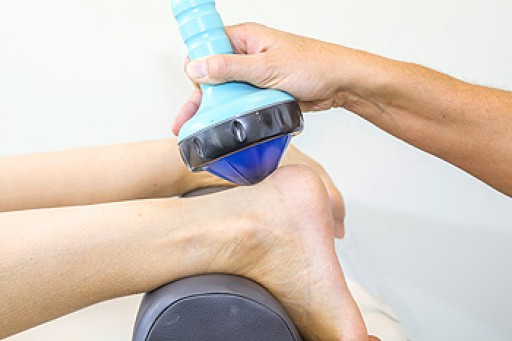
Shockwave Therapy is an emergent treatment of foot and ankle pain. In the United States, this innovative therapy has been licensed to treat plantar fasciitis: an inflammatory disorder in the tissue connecting the heel bone to the toes which causes pain in the heel. Shockwave Therapy—similar to Shockwave Lithotripsy for kidney stones—sends high-energy acoustic sound waves to the affected tissues at the bottom of the foot, which can initiate new blood vessel formation to begin the healing process and reduce pain. If you are experiencing pain in your heel or have been diagnosed with plantar fasciitis, call your podiatrist for more information or to see if you are a good candidate for Shockwave Therapy.
Shockwave therapy is a treatment commonly used to treat various injuries and conditions, particularly plantar fasciitis in the feet. To learn more, consult with one of our podiatrists from Canonsburg Podiatry Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Shockwave Therapy
Shockwave therapy is a new treatment option designed to treat bone conditions such as tennis elbow, shoulder pain, and others. Shockwave therapy uses high intensity sound waves that are directed to the affected tissues of the body with pinpoint accuracy. The effects are very beneficial, leading to a production of collagen fibers, eliminating inflammation.
Who Benefits from Shockwave?
Shockwave is recommended for patients suffering from heel pain and associated problems. Heel pain is a common condition which can be caused by obesity, overexertion, and spending a substantial amount of time on hard floors with your feet exposed and unsupported.
Fast and Easy
The therapy is actually a simple process that can leave patients feeling better the very next day. Shockwave therapy is not as dramatic as it sounds. It enables more blood flow to effected areas, addressing the source of the problem and allowing treatment to last for a long time.
Treatment & Recovery Time
Shockwave treatment will enable your feet to recover quickly. This is especially important since surgery is not required. It is cost effective and does not require the use of anesthesia. This treatment is a better option to surgery, since it is proven safe.
If you have any questions, please feel free to contact our office located in Canonsburg and McMurray, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.